aged care
In-Home Healthcare for Older Australians: Complete Guide

Why Home-Based Care Makes Such a Difference
The research on this is consistent. A August 2025 narrative review published in the Medical Journal of Australia by researchers at Flinders University and the South Australian Health and Medical Research Institute examined the evidence for models of care that support older people to age in place. The review found that while high-quality evidence remains an area of ongoing development, complex multifactorial, person-centred models of care that include comprehensive assessment and care planning—and that address both health and social needs—were the most consistently associated with helping older people remain in their homes [2]. A related finding from the same review was striking: an Australian study of more than 69,000 older people receiving home-based aged care found those who were least frail had a 10% lower likelihood of transitioning to residential long-term care when they received GP-led comprehensive geriatric assessment as part of their care [2].
For people living with dementia, the benefits of familiar surroundings are particularly well-documented. Established routines provide cognitive anchoring. Family involvement remains natural and continuous. These are not small things. They are the building blocks of quality of life.
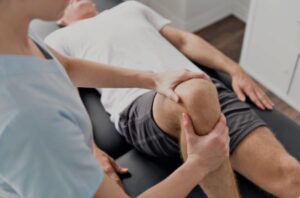
The therapists on our network report something similar time and again: when they visit clients in their own homes, they see a different person than they might in a clinic. People are more relaxed, more communicative, and more engaged in their own recovery. That confidence translates directly into better therapeutic outcomes.
Home-based care also supports something that clinical settings often inadvertently undermine: dignity. There’s no waiting room. No unfamiliar faces. No disruption of the rhythm that gives a person’s day meaning. For older Australians who may already feel a loss of control over aspects of their lives, being cared for at home restores agency in a way that genuinely matters.
Recognising When In-Home Support Might Be Needed
One of the harder conversations families face is recognising when things have shifted. It rarely happens all at once. More often, it’s a gradual accumulation of small signs that, taken together, suggest someone needs more support than they’re currently getting.
Here are some things worth paying attention to:
- Missed or muddled medications. This is one of the most common and consequential warning signs. If you’re noticing that a parent or loved one is forgetting their medications, taking incorrect doses, or becoming confused about their regimen, that warrants attention. A home-visiting nurse or pharmacist can conduct a medication review and put systems in place.
- Falls or near-misses. Falls are the leading cause of hospitalised injuries and injury deaths among older Australians, costing more than $2.8 billion annually and resulting in approximately 400 hospital admissions every single day [3]. A fall doesn’t have to be dramatic to be significant. If someone is holding walls more than they used to, hesitating at steps, or has had even one unexplained fall, a physiotherapist or occupational therapist visiting at home can assess both the person and their environment. The 2025 Australian fall prevention guidelines from the Australian Commission on Safety and Quality in Health Care emphasise individualised exercise programs, home safety interventions, and medication reviews as the core evidence-based response [4].
- Declining mobility or increasing pain. If getting around the house has become harder, or if pain is limiting activity, a mobile physiotherapist can assess and treat in the environment where those challenges actually occur—which is far more useful than a clinic assessment that doesn’t account for the person’s specific floor surfaces, furniture layout, or bathroom setup.
- Changes in mood or social withdrawal. Isolation is one of the most significant health risks for older Australians. A 2025 study using data from more than 12,000 community-dwelling Australians over 70 years of age found that persistent loneliness was associated with a significantly greater risk of dementia—with the effect particularly pronounced in women, where those who experienced ongoing loneliness had more than double the dementia risk of those who were never lonely [5]. Broader research confirms that social isolation increases the risk of premature death by approximately 29% [6]. A psychologist or counsellor who visits at home can provide support without the barrier of travel and unfamiliar settings.
- Difficulties with daily tasks. Struggling to cook, manage personal hygiene, or maintain the home safely can point to a need for occupational therapy support, care coordination, or both.
Families who use our platform tell us that they often wish they had asked for help sooner. There is no shame and no failure in recognising that someone you love needs more support. Asking for it is an act of care.
What Services Can Be Delivered at Home?
The range of healthcare that can now be delivered in the home is genuinely impressive. This is not second-rate care. These are fully qualified practitioners providing the same clinical services they would in a clinic, adapted to a home environment.
- Nursing. Registered and enrolled nurses can provide wound care, medication management, health monitoring, post-surgical care, and chronic disease management in the home. For older Australians managing complex conditions, having a nurse visit regularly can dramatically reduce unnecessary hospital visits.
- Physiotherapy. Mobile physiotherapists work with older adults on falls prevention, rehabilitation after surgery or injury, strength and balance programmes, pain management, and neurological conditions including stroke recovery and Parkinson’s disease. A 2025 randomised controlled trial published in the Medical Journal of Australia evaluated the TOP-UP (Telephysiotherapy for Older People) program and found that participants who received a six-month telephysiotherapy exercise program had fewer falls, and showed improvements in sit-to-stand performance, balance, gait speed, and quality of life—with 94% saying they would recommend the approach to others [7]. This evidence supports physiotherapy programs for older adults as clinically meaningful whether delivered in-person or in hybrid form.
- Occupational Therapy. OTs are perhaps the most practically powerful practitioners in the in-home space. They assess how someone functions in their own environment and recommend modifications, aids, and strategies that allow continued independence. A home visit OT can identify a bathroom hazard, recommend a grab rail, and arrange its installation—all in a single visit. Under the Support at Home Program, occupational therapy assessments are used to access the Assistive Technology and Home Modifications pathway, which provides a separate budget specifically for equipment and home modifications.
- Podiatry. Foot health is critically important for older Australians and is often overlooked. Untreated foot conditions contribute to falls, reduced mobility, and serious complications for people with diabetes. A mobile podiatrist brings the same clinical skill as a clinic-based practitioner, without requiring the person to travel.
- Audiology. Hearing loss affects a large proportion of older Australians and is now identified by the 2024 Lancet Commission as the single largest modifiable risk factor for dementia from mid-life. Mobile audiologists can conduct assessments at home, assist with hearing aid fitting and management, and make a real difference to someone’s ability to engage with their world.
- Speech Pathology. Swallowing difficulties (dysphagia) are common in older adults, with a 2024 systematic review and meta-analysis finding a pooled prevalence of over 56% among people in residential aged care settings [8]. Dysphagia can be life-threatening if unmanaged, leading to aspiration pneumonia, malnutrition, and dehydration. Speech pathologists also support people with communication difficulties, including those arising from stroke or dementia. In-home visits allow the speech pathologist to observe mealtimes and communication in real context—something a clinic visit cannot replicate.
- Psychology and Mental Health Support. Access to mental health support has historically been one of the hardest services for housebound Australians to access. Mobile psychologists and counsellors are changing that. For someone dealing with anxiety, depression, grief, or adjustment to a new diagnosis, the ability to access professional support without leaving home removes a significant barrier.
- Dietetics and Nutrition. Malnutrition is significantly underrecognised in older Australians—with estimates suggesting up to 50% of people in residential aged care settings experience it, despite having regular meals provided. A mobile dietitian can assess nutritional status, review eating patterns and food preparation in the actual kitchen, and provide practical, personalised advice. Where dysphagia is also present, dietitians and speech pathologists work closely together to ensure safe eating while maintaining adequate nutrition.
Understanding the Support at Home Program
The Australian Government’s Support at Home Program launched on 1 November 2025, replacing the previous Home Care Packages and Short-Term Restorative Care programmes under the new Aged Care Act 2024 [9]. This is the most significant structural change to aged care funding in decades, and understanding how it works is essential for families trying to act on any of the guidance in this article.
How the funding structure works
Support at Home uses eight funding classifications (replacing the previous four Home Care Package levels), with annual budgets indexed from approximately $10,700 (Classification 1) to $78,106 (Classification 8) per year, depending on assessed care needs. Annual funding is divided into four quarterly budgets—released in January, April, July, and October—giving participants clearer visibility and more flexibility in planning their care across the year.
Providers are subject to a capped 10% care management fee deducted from each quarterly budget, ensuring at least 90% of every quarter’s funding reaches direct services. If a participant does not spend their full quarterly allocation, they can carry over unspent funds to the next quarter, up to $1,000 or 10% of that quarter’s budget, whichever is higher—this happens automatically [9].
Services are grouped into three categories with different funding rules:
- Clinical care (nursing, physiotherapy, OT, speech pathology, and other allied health): fully funded by the government — participants pay no out-of-pocket contribution
- Independence services (personal care, social support): moderate participant contributions apply based on income and assets
- Everyday living services (domestic assistance, transport, meals): highest participant contributions apply
The Assistive Technology and Home Modifications Scheme
Support at Home also includes a separate Assistive Technology and Home Modifications (AT-HM) Scheme—a distinct funding stream specifically for equipment, aids, and home modifications such as grab rails, ramps, shower chairs, and personal alarms. AT-HM funding is held separately from the quarterly budget and is valid for 12 months. For people transitioning from Home Care Packages who had unspent funds, those retained funds must be used for AT-HM purposes first before accessing the AT-HM Scheme [9]. Occupational therapy assessments are typically used to identify and justify AT-HM needs.
The access reality families need to know
One thing families must understand before starting this process: the current waitlist is severe. As of September 2025, 121,909 people were on the National Priority System waiting for funding at their approved level—a 26% increase in just three months—with a combined backlog likely exceeding 200,000 when those still awaiting assessment are included [10]. Median wait times for approved applicants stretch to nine to eleven months. Expert modelling projects the waitlist could reach 300,000 by 2030 [10]. Interim funding (typically 60% of the approved quarterly budget) is available for eligible applicants while they wait for full classification. The practical message: start the process early, before a crisis forces urgency.
How to access funding
Contact My Aged Care to request an assessment through the Single Assessment System (which replaced ACAT and RAS on 9 December 2024 [10]). After assessment and classification, you choose an approved provider. Some services can also be accessed independently of Support at Home: Medicare provides rebates for up to five allied health visits per calendar year under a GP Chronic Condition Management Plan (GPCCMP, from 1 July 2025), and DVA cardholders may access allied health through DVA arrangements.
If you receive CHSP services
The Commonwealth Home Support Programme has been formally extended through to 30 June 2027 and will not merge into Support at Home until that date at the earliest. However, from 1 November 2025 all CHSP clients are required to be registered through My Aged Care and have a formal aged care needs assessment on file to continue receiving government-subsidised services under the new Act [9]. Most existing clients were automatically transitioned, but if you or a family member has been receiving CHSP services without a formal assessment, contact your provider or My Aged Care promptly to confirm your registration status.
Your Rights Under the New Act
The Aged Care Act 2024, which commenced on 1 November 2025 alongside Support at Home, is a rights-based law that fundamentally changes the legal footing of every older Australian in the system. At its centre is a Statement of Rights—codified in section 23 of the Act—which includes legally enforceable rights to independence and autonomy, culturally safe and trauma-informed care, freedom from abuse, neglect and discrimination, and the right to raise complaints without fear of reprisal [11]. Providers are legally obliged to deliver services in a manner compatible with these rights.
The Act also establishes an independent Complaints Commissioner within the Aged Care Quality and Safety Commission, with the authority to investigate complaints, issue required action notices to providers, and enforce outcomes [11]. If a concern cannot be resolved with a provider directly, it can be escalated to the Complaints Commissioner. Free, independent advocacy is available through the Older Persons Advocacy Network (OPAN) on 1800 700 600. These protections apply to all older Australians accessing government-funded aged care services, including in-home care.
Finding the Right Practitioner
Choosing a mobile healthcare professional involves more than finding someone in your postcode. For older Australians and their families, it’s worth asking specifically about experience with home visits, comfort working in aged care environments, and familiarity with government funding pathways including Support at Home and DVA.
It also matters how the practitioner approaches the rest of your care team. Mobile practitioners who work well in home settings tend to be confident communicators who can write reports, share assessments, and coordinate with GPs and specialists. That collaborative approach is often what makes the difference between a one-off visit and a care plan that actually holds together.
You can find qualified mobile practitioners who service your area by conducting a postcode search on the Home Visit Network platform.
A Note for Carers and Family Members
We want to speak directly to you for a moment, because this guide is as much yours as it is your loved one’s.
Caring for an ageing parent or partner is one of the most demanding roles a person can take on. The physical demands are real. The emotional weight is substantial. And the administrative burden of navigating the aged care system can feel relentless.
Bringing professional support into the home is not giving up. It is, in fact, one of the most sustainable things you can do for both of you. Carers who access professional support for their loved ones report lower rates of burnout, and the people they care for report better health outcomes. That is a good trade.
If you’re not sure where to start, start with a conversation. Talk to the GP. Call My Aged Care on 1800 200 422. And when you’re ready to find a practitioner who visits the home, conduct a postcode search on the Home Visit Network platform to see who is available in your area.
Frequently Asked Questions
What types of healthcare professionals can visit me at home?
A wide range of qualified practitioners can provide services in the home, including registered nurses, physiotherapists, occupational therapists, podiatrists, audiologists, speech pathologists, psychologists, and dietitians. The range has expanded significantly in recent years as demand for in-home care has grown.
How do I find out if I’m eligible for government-funded in-home care?
The starting point is My Aged Care (myagedcare.gov.au or 1800 200 422). An aged care assessment through the Single Assessment System (which replaced ACAT from 9 December 2024) will determine your eligibility and level of need. Some allied health services may also be accessible through a Medicare GP Chronic Condition Management Plan (GPCCMP) via your GP.
Can I access in-home healthcare without Support at Home funding?
Yes. Allied health services are available through Medicare with a GP referral under a GPCCMP, through DVA for eligible veterans, or through private payment. A GP is a good first point of contact to understand what is available and what is funded.
What is the Support at Home Program and how does it affect me?
The Support at Home Program launched on 1 November 2025, replacing Home Care Packages. It has eight funding classifications with annual budgets from $10,700 to $78,106, delivered as quarterly budgets with a capped 10% care management fee. Clinical care including allied health is fully government-funded at no out-of-pocket cost. A separate AT-HM Scheme funds equipment and home modifications. Unspent quarterly funds carry over automatically up to $1,000 or 10% of your budget. More information: myagedcare.gov.au.
How do I find a mobile healthcare professional in my area?
You can find qualified mobile practitioners by conducting a postcode search on the Home Visit Network platform. All practitioners on the platform are registered with their relevant professional bodies.
What if my loved one is resistant to accepting help?
This is very common. Often the most effective approach is to start with a single, specific, low-stakes service rather than a broad conversation about “getting help.” A physio to address a specific pain, or a podiatrist for foot care, can open the door. Practitioners experienced in working with older adults are skilled at building trust gradually.
References
- Alsaeed T, Washington T, et al. Comprehensive analysis of Australia’s aged care system to inform policies for a sustainable future. Frontiers in Public Health. 2025. doi: 10.3389/fpubh.2025.1525988
- Inacio MC, Harrison S, Schwabe J, et al. Models of care across settings supporting ageing in place: a narrative review. Medical Journal of Australia. 2025;223(4):218–225. doi: 10.5694/mja2.70003
- Delbaere K, Sherrington C, Said CM, et al. Innovative approaches to fall prevention in community-dwelling older adults. Medical Journal of Australia. 2025;223(4):174–176. doi: 10.5694/mja2.52714
- Australian Commission on Safety and Quality in Health Care. Preventing falls and harm from falls in older people: Best practice guidelines for community care. 2025. safetyandquality.gov.au
- Htun HL, Teshale AB, et al. Changes in loneliness, social isolation, and social support: a gender-disaggregated analysis of their associations with dementia and cognitive decline in older adults. International Journal of Geriatric Psychiatry. 2025;40(3):e70065. doi: 10.1002/gps.70065
- Holt-Lunstad J, et al. Loneliness, social isolation, and living alone: a comprehensive systematic review, meta-analysis and meta-regression of mortality risks in older adults. Aging Clinical and Experimental Research. 2025. doi: 10.1007/s40520-024-02925-1
- Dawson R, Pinheiro M, Oliviera J, et al. The Telephysiotherapy for Older People (TOP-UP) program for improving mobility in people receiving aged care: a hybrid type 1 effectiveness-implementation randomised controlled trial. Medical Journal of Australia. 2025;223(4):205–213.
- The prevalence of dysphagia in individuals living in residential aged care facilities: a systematic review and meta-analysis. PMC. 2024. doi: 10.3390/healthcare12060614
- Australian Government Department of Health, Disability and Ageing. Support at Home Program. Commenced 1 November 2025. health.gov.au
- Australian Government Department of Health, Disability and Ageing. Single Assessment System for aged care. Commenced 9 December 2024. health.gov.au
- YourLifeChoices; The Weekly Source. Home care waitlist surges to 121,909—up 26% in three months. October 2025. Aged Care Made Easy. Support at Home wait times Australia 2026. agedcaremadeeasy.com.au
- Older Persons Advocacy Network (OPAN). New Aged Care Act: Statement of Rights and independent complaints process. Updated 1 November 2025. opan.org.au; MinterEllison. Aged Care Act 2024: complaints, whistleblower and feedback regime. minterellison.com